Post-Arrest STEMI: Cath Lab or Caution?
Emergency Cardiology Literature Review & Updates with Dr. Amal Mattu
HPI
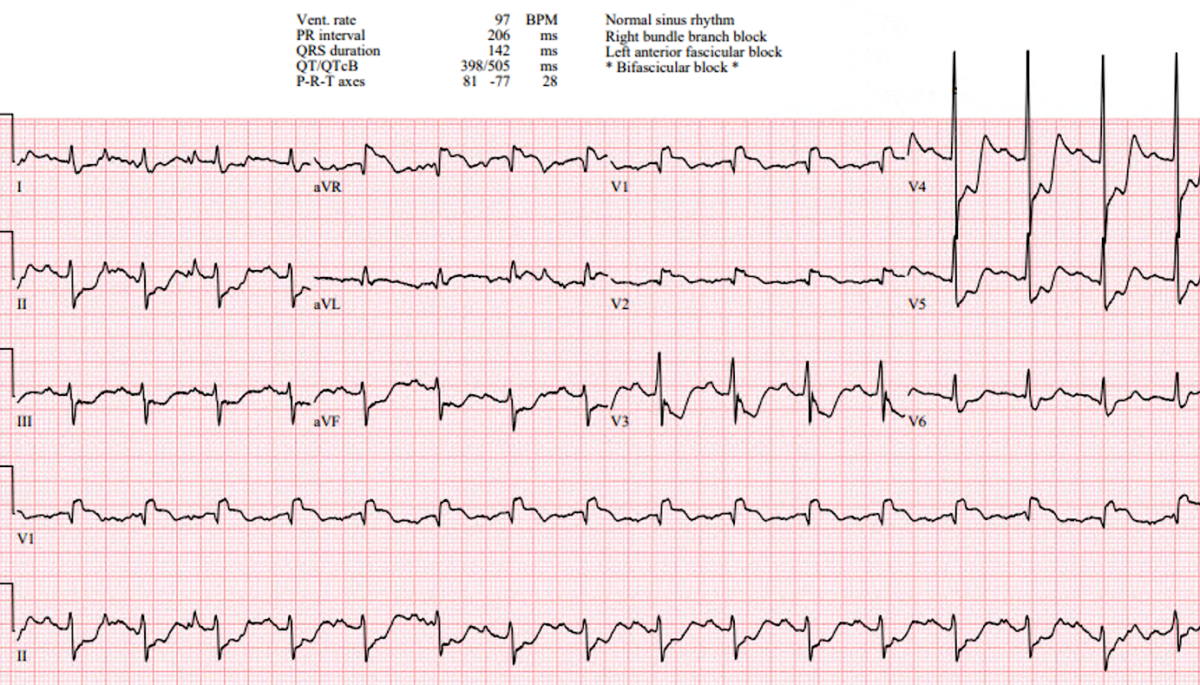
A 72-year-old man is brought to the ED after witnessed cardiac arrest. Bystander CPR was started quickly, EMS found a nonshockable rhythm, epinephrine was given, and ROSC was achieved. Forty minutes later, the patient remains comatose, and the ECG shows new septal ST elevation with new bifascicular block and reciprocal changes. This week’s ECG Weekly Workout moves beyond the tracing and into the decision that follows: should a comatose post-arrest STEMI patient still go immediately to the cath lab?
Questions to consider:
-
- How should you interpret persistent ST elevation 40 minutes after ROSC compared with ST changes seen immediately after ROSC?
- What “unfavorable resuscitation features” should influence the cath lab discussion, and how should they be weighed?
- Does the MIRACLE2 score change management, or does it mainly help structure the prognosis conversation?